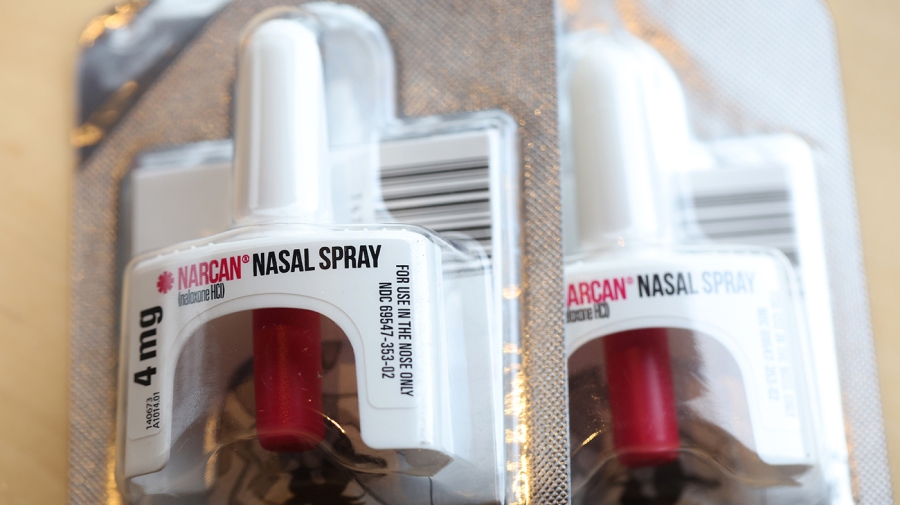
The Food and Drug Administration’s move to make a version of naloxone available without a prescription marks a major milestone in the fight against opioid addiction, and anti-addiction advocates hope it will break down barriers and help expand access to the drug.
The agency approved Narcan, the brand-name nasal spray manufactured by Emergent BioSolutions. But the company did not say how much it will charge, and there is concern that unless it is priced affordably, over-the-counter Narcan will likely have little impact on the people who need it most.
The change from prescription to over-the-counter has been a long time coming. Until now, all versions of naloxone have been available by prescription only. The agency has been encouraging companies to apply to sell their products over the counter since 2016, but no manufacturer applied until last year.
Naloxone is a medicine that can help reduce opioid overdose deaths and when administered timely, usually within minutes of the first signs of an opioid overdose, can counter the overdose effects.
“FDA’s announcement to make Narcan available over the counter is an important step to make this medicine accessible to more people at a time when the majority of overdose deaths are being driven by illicit opioids like fentanyl,” said Rahul Gupta, director of the White House Office of National Drug Control Policy.
The nearly 107,000 fatal overdoses reported in 2021 were primarily driven by synthetic opioids like illicit fentanyl. With naloxone, many of those deaths could have been avoided.
FDA Commissioner Robert Califf in a statement encouraged Emergent to make the drug available “at an affordable price.”
The retail cost of prescription Narcan varies, but after discounts a two-pack of Narcan is around $45 to $50. For people with insurance coverage, it can be even cheaper.
Yet health insurance plans don’t typically cover over-the-counter drugs, so there’s a chance FDA’s move could make Narcan more expensive than it already is.
“All payers must continue or start to cover naloxone at no- or low-cost. There are many over-the-counter preventive health medications that are covered by insurance, such as aspirin, vitamin D, and fluoride. Naloxone should be added to that list,” Bobby Mukkamala, chair of the American Medical Association’s Substance Use and Pain Care Task Force, said in a statement.
Sarah Wakeman, medical director for substance use disorder at Massachusetts General Hospital Brigham, said the ideal vision would be for Narcan to be sold not just at pharmacies but at gas stations, convenience stores and in vending machines.
“If you’re walking through subway stations, if you’re on the street, if you know and love someone who uses drugs, you should have this in your backpack, in your purse,” Wakeman said.
But she acknowledged that the price translates directly into where those stores will put the product. If there’s a worry people will shoplift Narcan, or if stores decline to carry it because of concerns they’ll be promoting drug use, it won’t be nearly as accessible.
“I think the goal should be to make this as easy as possible for people to access … if it’s behind the counter, or if it’s in sort of a locked glass box where you have to ask someone for help, that’s going to be one more hurdle and especially for someone who’s dealing with the stigma that’s unfortunately still associated with drug use in this country,” Wakeman said.
Eliza Wheeler, co-director of the nonprofit group Remedy Alliance/For The People, said the hope is that making Narcan available over-the-counter will eliminate some of the “bureaucratic gatekeeping” that prevents harm reduction groups from purchasing and distributing Narcan.
For example, some state laws specify that only a medical professional can distribute naloxone to the community because it is a prescription drug. If the drug is no longer a prescription medication, those rules and regulations will go away.
“But, you know, our primary focus is always cost. And so if cost doesn’t go down, that accessibility is going to stay limited,” Wheeler said.
Wheeler’s group is a wholesaler that negotiates with pharmaceutical companies for generic injectable naloxone; the group then sells the drug at extremely reduced rates to harm reduction programs.
According to FDA, prescription Narcan is currently the most commonly sold emergency treatment for opioid overdose in United States pharmacies. It was first approved in 2015 to treat known or suspected opioid overdoses for people of all ages, including newborns.
More than 44 million doses of Narcan have been distributed since its launch in 2016, the company said.
All 50 states have found workarounds to make the drug available at the pharmacy without a prescription through what’s known as “standing orders” — essentially blanket prescriptions that allows pharmacists to dispense naloxone to anyone at risk or in a position to assist someone at risk.
Yet the people who need naloxone the most are also the least likely to go to a pharmacy and request it.
The cost of the medication, requirements to show ID, and the overall stigma of asking for naloxone are all barriers. Additionally, some pharmacists may not be aware that there is a standing order in their state and refuse to prescribe the drug altogether.
Susan Bissett, president of the West Virginia Drug Intervention Institute, said Narcan is just one product, but she hopes making it available without a prescription will mark a turning point for widespread public accessibility of naloxone.
“Business as usual is not getting the job done,” Bissett said. “We’re no longer just talking about people in active addiction. We’re talking about kids on college campuses who are taking counterfeit Adderall pills that are laced with fentanyl … we’re hearing reports of kids overdosing in schools from vape pens because they’re laced with fentanyl. So we’re dealing with a completely different opioid epidemic than what we were 10 years ago.”